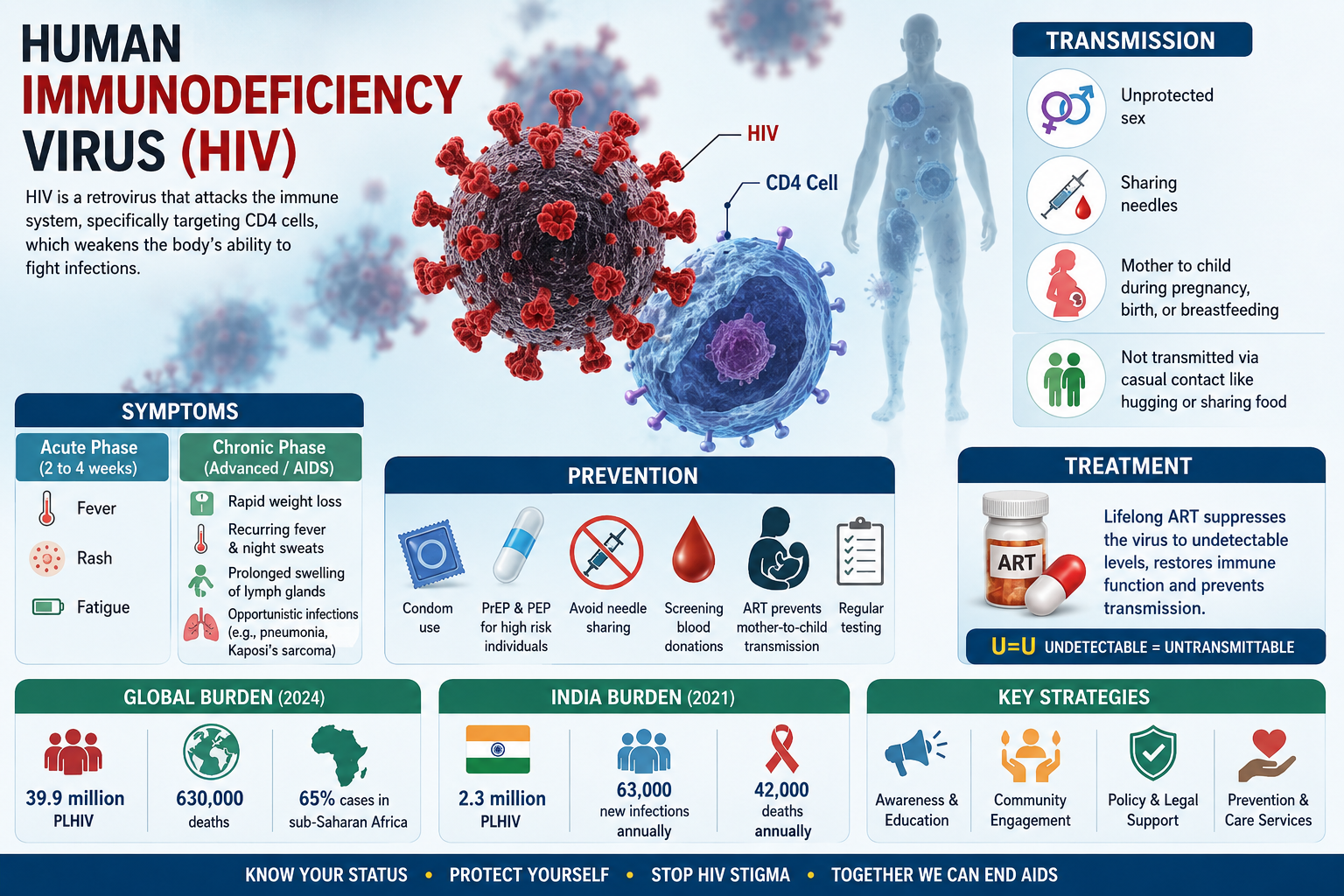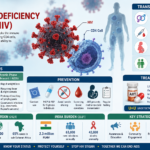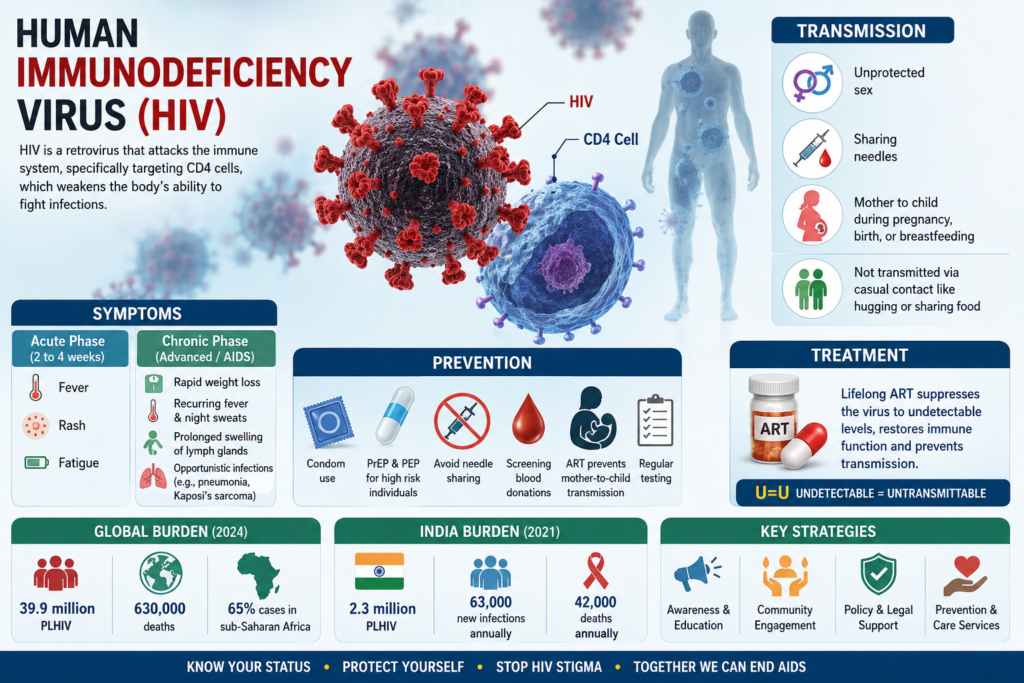
Human Immunodeficiency Virus (HIV) is a retrovirus that attacks the immune system, specifically targeting CD4 cells, which weakens the body’s ability to fight infections.
Definition
Human Immunodeficiency Virus (HIV) causes progressive immune deficiency, potentially leading to Acquired Immunodeficiency Syndrome (AIDS) if untreated. AIDS represents the advanced stage where opportunistic infections and cancers thrive due to severe immune damage.
Transmission
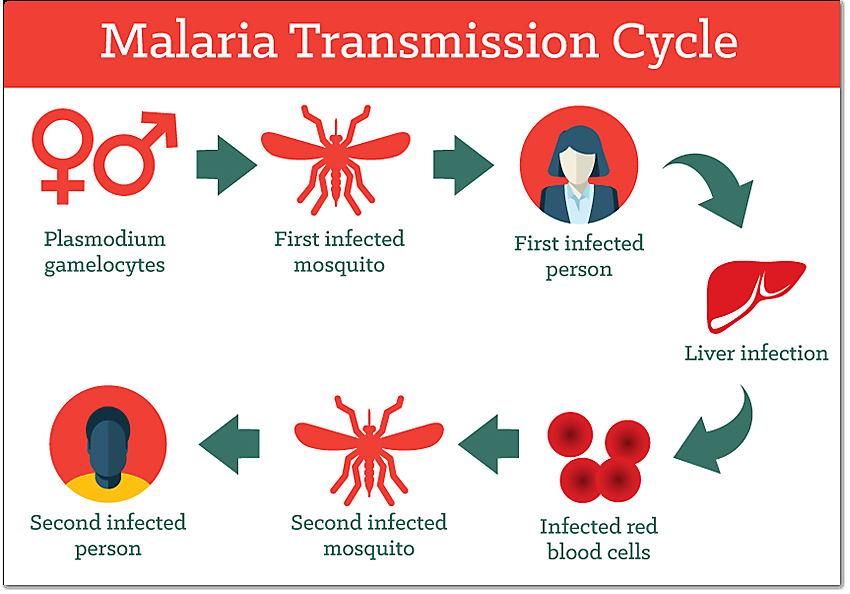
HIV spreads through specific body fluids like blood, semen, vaginal fluids, rectal fluids, and breast milk from infected mothers.
Common routes include unprotected sex, sharing needles, and mother to child during pregnancy, birth, or breastfeeding; it does not transmit via casual contact like hugging or sharing food.
Main Types
HIV-1
Most common globally, highly virulent, responsible for the majority of infections.
HIV-2
Less transmissible and progresses slower, mainly in West Africa.
Symptoms
Acute Phase (Early Infection)
(2 to 4 weeks post-infection); may cause flu-like symptoms such as fever, rash, and fatigue.
Chronic Phase
Followed by a long asymptomatic period.
In AIDS, symptoms include rapid weight loss, recurring fever, night sweats, extreme fatigue, prolonged swelling of lymph glands, and opportunistic illness like pneumonia or Kaposi’s sarcoma.
Diagnosis
Diagnosis confirms HIV infection via blood or saliva tests detecting antibodies, antigens, or viral RNA; it’s typically done after risk exposure or routine screening.
Diagnosis Methods
Antibody Test (ELISA, Rapid Tests)
Detect immune response (window period 23 to 90 days).
Antigen/Antibody Tests
Earlier detection (18 to 45 days).
Nucleic Acid Tests (NAT)
Detect virus directly (10 to 33 days), used for infants or high-risk cases.
Prevention
Key strategies include condom use, pre-exposure prophylaxis (PrEP) for high-risk individuals, and post-exposure prophylaxis (PEP) within 72 hours.
Avoiding needle sharing, male circumcision, screening blood donations, and regular testing.
Antiretroviral therapy (ART) prevents mother-to-child transmission.
Control Measures
Antiretroviral therapy (ART) to suppress viral load, contact tracing, safe sex promotion, harm reduction for drug users, and mother-to-child transmission prevention via ART during pregnancy.
Treatment
Lifelong ART—a combination of antiretrovirals like nucleoside reverse transcriptase inhibitors suppresses the virus to undetectable levels, restoring immune function and preventing transmission (“U=U”—undetectable + untransmittable); no cure exists.
Public Awareness
Campaigns educate on transmission myths, testing importance, and stigma reduction through media, schools, and community programs to encourage safe behaviors and early diagnosis.
Community Engagement
Involves NGOs, peer educators, support groups for PLHIV, and key populations (e.g., MSM, sex workers) to promote testing, adherence, and advocacy against discrimination.
IEC Materials
Information, education, and communication tools like posters, pamphlets, videos, and apps in local languages on prevention, testing sites, and ART benefits, distributed via health centers and media.
Role of Public Health Department
Leads surveillance, provides free testing/ART via NACO/State AIDS Control Societies, runs awareness drives, ensures supply chains, monitors epidemics, and integrates HIV into general health services.
Magnitude
Chronic, incurable infection affecting 39 million globally in 2024, with 1.3 million new cases yearly.
Global Burden
39.9 million PLHIV (2024 est.), 630,000 deaths; sub-Saharan Africa bears 65% of cases; progress via ART access but gaps in prevention.
Burden in India
The third highest globally: 2.3 million PLHIV (2021), adult prevalence ~0.22%, 63,000 new infections, 42,000 deaths annually, high in key populations, 77% diagnosed, 65% on ART.
Burden in Maharashtra
High prevalence state: Among the top for MSM (13% prevalence in 2021-11 surveys); significant urban/rural cases, focused interventions via state AIDS society.
HIV Statistics and Prevalence Trends in India, 2026
India has made significant strides in controlling HIV, with adult prevalence stable at around 0.20% and a large but managed burden of people living with HIV (PLHIV).
Key Statistics 2024
India has an estimated 2.56 million people living with PLHIV as of 2024, making it the second highest globally HIV burden after South Africa, including 1.40 million males and 1.16 million females.
New infections are approximately 645,000 annually, and AIDS-related deaths are approximately 32,000.
Prevalence Trends
Adult HIV prevalence held at 0.20% in 2024, down from higher rates pre-2010; annual incidence rate is very low at 0.05 per 1000 uninfected population.
From 2010 to 2024: new infections declined 48.7%. AIDS deaths dropped 81.4%, and mother-to-child transmission fell 74.6%.
State-wise Burden
Top states account for 74%: Maharashtra (399,000 PLHIV), Andhra Pradesh (310,000), and Karnataka (291,000); these nine states account for 74% of the total burden.
High mortality in Manipur, Mizoram, and Nagaland; rising new infections in northeastern states like Tripura, Arunachal Pradesh, Meghalaya, Assam, and Punjab.
Treatment and Testing Progress
ART coverage rose from 1.49 million (pre-2024) to 1.86 million PLHIV.
HIV testing from 41.3 million (2020-21) to 66.2 million (2024-25).
Viral load tests from 0.89 million to 1.60 million.
Transmission Breakdown (2024-25 New Cases)
Heterosexual: 73%; injecting drug use, homosexual/bisexual: 5.4%; and vertical: 3.5% cases are found.
HIV Prevention Strategies in India
India implements multifaceted HIV prevention strategies through the National AIDS Control Programme (NACP), focusing on high-risk groups and general population awareness.
Targeted Interventions (TI)
Peer-led programs for key populations like female sex workers, men who have sex with men (MSM), transgender persons, and people who inject drugs (PWID).
Include behavior change communication, condom promotion, STI services, needle-syringe exchange, and opioid substitution therapy.
Condom Promotion
Free condom distribution via social marketing and targeted campaigns: over 6 billion condoms supplied annually to promote consistent use in high-prevalence areas.
Pre-Exposure Prophylaxis (PrEP)
Oral PrEP (tenofovir disoproxil fumarate/emtricitabine) rolled out for high-risk serodiscordant couples and key populations since 2017, with scale-up in demonstration projects.
Mother-to-child Transmission Prevention
Universal antiretroviral therapy (ART) for pregnant women living with HIV, syphilis co-testing for 30+ million annually, and comprehensive PMTCT services at 740 ART centers.
Testing and Linkage to Care
Provider-initiated testing, self-testing kits, and community-based screening; the “test and treat” policy since 2017 ensures immediate ART initiation regardless of CD4 count.
Awareness and Education
Red Ribbon Clubs in 14,000+ colleges, adolescence education programs in schools, folk media reaching millions, and mass events like RED RUN marathons to combat stigma.
Policy and Legal Support
The HIV and AIDS (Prevention and Control) Act 2017 prohibits discrimination, mandates ombudsmen in states, and integrates HIV with TB/hepatitis programs.