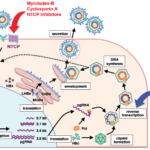
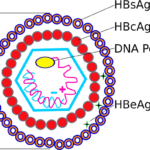
The hepatitis B virus (HBV) has a relatively simple but highly organized structure centered around a small DNA-containing core wrapped in an envelope.
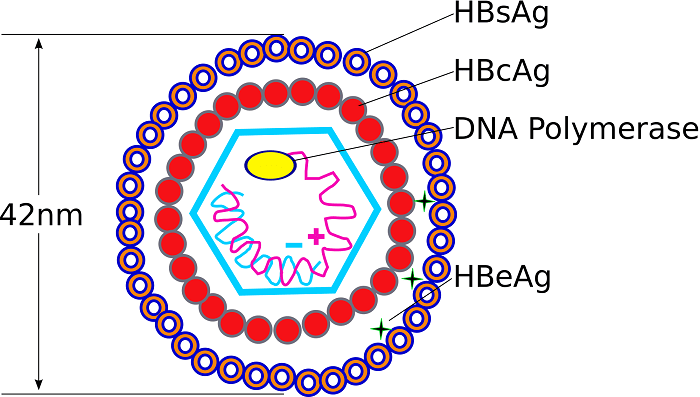
Overall Particle Forms
Dane Particle (42 nm)
Dane particle (42 nm): The complete, infectious virion; about 42 nm in diameter, with an outer lipid envelope and an inner icosahedral nucleocapsid.
Subviral Particles
Subviral particles: 22 nm spherical particles and tubular filamentous particles (~22 nm), which are non-infectious and mainly made of surface antigen (HBsAg) produced in excess by the virus.
Key Structural Components
Outer Envelope (Surface Antigen, HBsAg)
Outer envelope (surface antigen, HBsAg): Composed of lipid and three types of surface proteins (S, M, and L variants) embedded in the membrane. These proteins bind to receptors on liver cells (hepatocytes) and are the main target of HBV vaccines and diagnostic tests.
Inner Nucleocapsid (Core Particle)
Inner nucleocapsid (core particle): Icosahedral core (~27 to 30 nm) made of hepatitis B core antigen (HBcAg) dimers that assemble into a shell. This core encloses the relaxed circular double-stranded DNA (rcDNA) and the viral DNA polymerase/reverse transcriptase, which performs reverse transcription inside the capsid.
HBeAg (Hepatitis B e Antigen)
HBeAg (Hepatitis B e antigen): A secreted protein derived from the same reading frame as HBcAg, closely associated with the core. It is not part of the virion structure but circulates in blood and is used clinically as a marker of high viral replication and infectivity.
In short, the key structures are: enveloped Dane particles → lipid envelope with HBsAg proteins → HBcAg capsid → rcDNA + DNA polymerase inside, plus the non-infectious subviral HBsAg spheres and filaments.
Role of HBsAg and HBcAg in Viral Infection
HBsAg and HBcAg are key viral proteins in hepatitis B virus (HBV) infection, but they play different roles in the virus life cycle and in the host immune response.
Role of HBsAg
Entry and Envelope Formation
Entry and envelope formation: HBsAg forms the outer lipid envelope of the virion; its S, M, and L surface proteins mediate binding to receptors on hepatocytes and allow the virus to enter liver cells.
Immune Evasion and Chronicity
Immune evasion and chronicity: Excess HBsAg in blood and on infected cell membranes dampens innate and adaptive immunity (for example, by suppressing plasmacytoid dendritic cell function), helping HBV establish and maintain chronic infection.
Diagnostic Marker
Diagnostic marker: HBsAg in serum is the hallmark of current HBV infection (acute or chronic); loss of HBsAg with the appearance of anti-HBs usually indicates resolution or a functional cure.
Role of HBcAg
Nucleocapsid and Genome Packaging
Nucleocapsid and genome packaging: HBcAg self-assembles into the icosahedral core (nucleocapsid) that encloses the viral DNA and reverse transcriptase and is essential for viral genome stability and replication inside the cell.
Gene Regulation and Nuclear Function
Gene regulation and nuclear function: HBcAg can enter the nucleus, bind to cccDNA (the viral mini-chromosome), and help regulate viral transcription and epigenetic modifications, thereby influencing the level of HBA replication.
Immune-Targeting Antigen
Immune-targeting antigen: HBcAg is a strong target for T-cell-mediated immunity; intrahepatic HBcAg expression correlates with liver inflammation and viral replication phase and is used as a prognostic marker for antiviral treatment response.
Thus,
- HBsAg mainly governs virus entry, envelope structure, and modulation of humoral/innate immunity and is the main blood marker of infection.
- HBcAg governs capsid formation, genome packaging, and nuclear regulation of viral genes and is a major driver of T-cell immune responses and liver-tissue pathology.
Diagnostic Importance of HBsAg and HBcAg in HBV
HBsAg and HBcAg are central to the diagnosis, staging, and monitoring of hepatitis B virus (HBV) infection, but they are used in different ways and in different compartments (blood vs. liver tissue).
Diagnostic Importance of HBsAg
Marker of Current HBA Infection
Marker of current HBA infection: HBsAg in serum is the primary screen for HBV; a positive HBsAg test means current infection (acute or chronic). If HBsAg persists for > 6 months, it defines chronic HBV infection as per guidelines.
Monitoring Treatment and Outcome
Monitoring treatment and outcome: Falling or declining quantitative HBsAg levels during interferon or nucleoside analog therapy are used to predict sustained response or functional cure. Loss of HBsAg with anti-HBs seroconversion is the best serological sign of resolution or functional cure.
Diagnostic Importance of HBcAg
Liver-Tissue Marker of HBV Activity
Liver-tissue marker of HBV activity: HBcAg in liver biopsy (by immunohistochemistry) identifies HBV-related hepatitis even when serum HBsAg is negative, helping to diagnose occult HBA or HBsAg-negative chronic hepatitis.
Patterns of HBcAg expression (nuclear vs. cytoplasmic) correlate with necro-inflammatory activity and fibrosis stage, aiding prognosis.
Link to Replication and Immune Phase
Link to replication and immune phase: High or specific HBcAg expression in hepatocytes usually indicates active viral replication and immune-mediated liver injury, useful for deciding when to start or change antiviral therapy.
Thus, HBsAg is the key blood marker for diagnosing and classifying HBV infection, while HBcAg in the liver helps define the etiology and intensity of hepatitis B-related liver disease, especially in HBsAg-negative or serologically ambiguous cases.