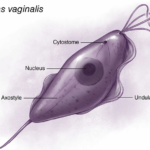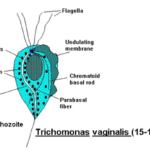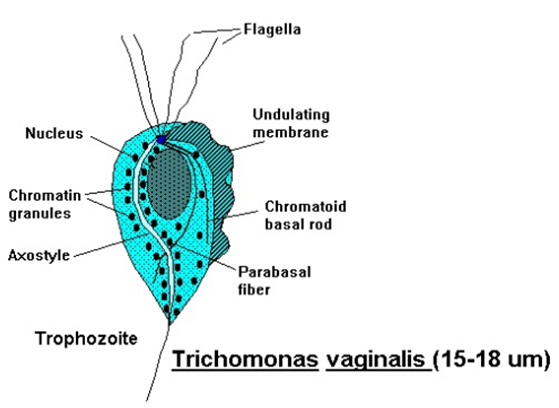
Trichomonas vaginalis exists solely as a trophozoite with no cyst stage, featuring a pear-shaped (pyriform) body typically 7 to 30 μm long and 5 to 15 μm wide.
External Features
Four anterior flagella emerge from a shared blepharoplast near the nucleus, enabling jerky motility, while a fifth flagellum runs along the outer edge of the undulating membrane, supported by the costa.
The undulating membrane spans about half the body length, aiding propulsion and attachment.
A prominent axostyle, a slender rod-like structure, runs longitudinally from the nucleus and protrudes posteriorly as a sharp point for anchoring to host cells.
Internal Structures
A single anterior nucleus with scattered chromatin granules and a small karyosome line at the broad end, enclosed by a porous nuclear envelope.
The cytoplasm contains hydrogenosomes (osmiophilic granules for energy via anaerobic metabolism), glycogen vacuoles, and hydrogenosomes arranged in rows along the axostyle.
Lysosome-like phagosomes and hydrolase enzymes support cytolysis and nutrient uptake.
Morphological Variants
In culture, trophozoites are pear- or oval-shaped; in vivo on vaginal epithelium, they adopt an amoeboid form with internalized flagella, reverting to active trophozoites when conditions improve.
Life Cycle of Trichomonas Vaginalis
Trichomonas vaginalis has a simple life cycle centered on its trophozoite form, the only well-established stage, which replicates directly in human hosts without a true cyst phase.
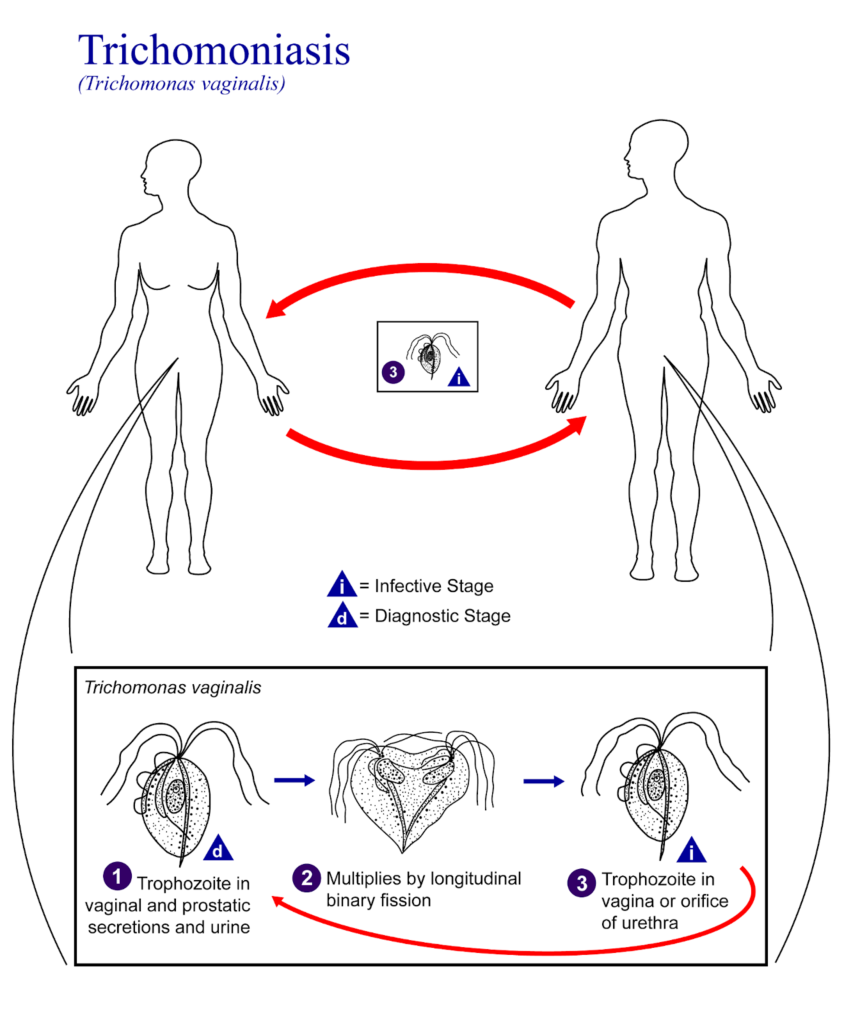
1) Core Life Cycle
The trophozoite, a pear-shaped, flagellated protozoan, lives in the female lower genital tract (vagina and cervix) or male urethra and prostate.
It multiplies by binary fission under favorable conditions like warmth and moisture.
Transmission occurs almost exclusively through sexual contact, as the parasite survives poorly outside the body, up to 24 hours in semen, urine, or water.
2) Morphological Adaptations
Trophozoites can shift to an ameboid shape to adhere to and lyse host epithelial cells during infection.
Under stress, they may form pseudocysts—rounded, nonmotile structures with internalized flagella that revert to trophozoites when conditions improve; these are not true cysts but aid survival.
Recent research suggests cyst-like structures (CLS) may enable non-sexual transmission, e.g., via fomites, co-existing with trophozoites in clinical samples.
3) Infection Dynamics
Incubation lasts 4 to 28 days, with infections persisting longer in women (months to years in crypts) than men (often < 10 days).
No intermediate hosts or environmental stages are involved; humans are the sole reservoir.
How Does Trichomonas vaginalis Attach to Host Cells?
Trichomonas vaginalis, a flagellated protozoan parasite causing trichomoniasis, attaches to host epithelial cells in the urogenital tract using specialized structures and mechanisms. Here’s a breakdown:
Adhesins and Surface Proteins
The parasite employs surface glycoproteins called adhesins, e.g., TvBspA, AP33, and AP65, that bind to host cell receptors like fibronectin, laminin, and mucin.
These proteins act like molecular “hooks,” enabling firm attachment.
Ultrastructural Features
It uses a pelta-uncus complex (hook-like organelle) and hydrogenosomes near the attachment site, which provide mechanical grip and energy for adhesion.
Microvilli-like extensions on the parasite surface interdigitate with host microplicae.
Dynamic Process
Attachment begins with flagella-mediated contact, followed by pseudopod formation for closer binding.
This can lead to endocytosis or membrane fusion, promoting infection.
Host-Parasite Interactions
Host galectins, e.g., galectin-1 and -3, are secreted in response; binding trophozoites’ lactose inhibits cluster formation on cell monolayers.
Adherent strains aggregate post-initial binding, showing a stronger correlation between attachment and host cell damage.
Morphology of Trichomoniasis
Trichomonas vaginalis morphology centers on its trophozoite form, the only stage in its life cycle, lacking true cysts.
It exhibits variable