HPV Vaccination.
HPV Vaccination Types and Recommended Ages
Main HPV Vaccine Types
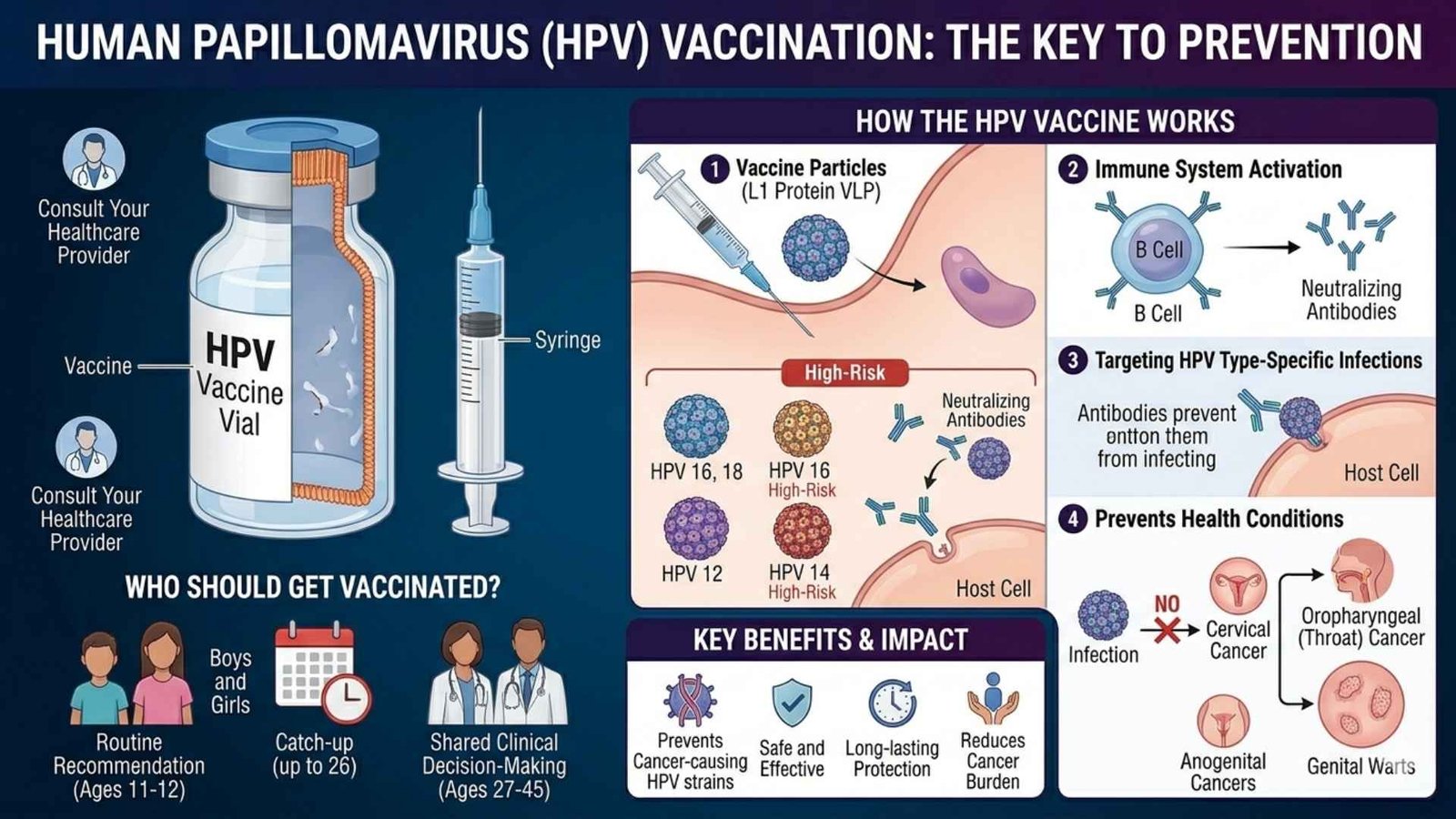
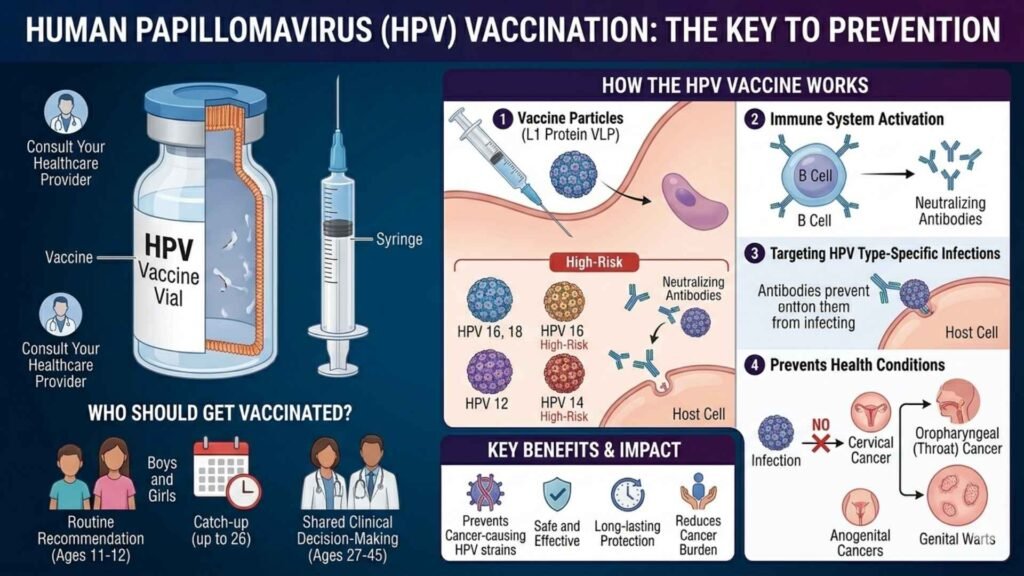
Globally, three main HPV vaccines are used; all are non-live, recombinant vaccines given as injections (usually in the arm).
Bivalent (2-valent) HPV Vaccine
Protects against HPV 16 and 18 (high-risk types causing most cervical cancers).
Quadrivalent HPV Vaccine (Gardasil-type)
Protects against HPV 6, 11, 16, and 18. Covers the two main cancer-causing types (16/18) plus 6/11 that cause most genital warts.
9-valent HPV Vaccine (Gardasil 9-valent / 9vHPV)
Protects against HPV 6, 11, 16, 18, 31, 33, 45, 52, and 58. Broadcast coverage prevents most HPV-related cervical, anal, vulvar, vaginal, penile, and oropharyngeal cancers and genital warts.
Recommended Ages and Schedule
Guidelines below follow WHO-aligned/CDC-type recommendations and are widely adapted in national programs (including India-style policies). India’s HPV vaccine rules focus on preventing cervical cancer through a nationwide program launched in late 2025. The program targets girls aged 14, providing free Gardasil quadrivalent vaccine at government facilities like Ayushman Arogya Mandirs and hospitals.
Routine Age Group (Best Age)
Target age: 11-12 years for both boys and girls (before sexual debut).
Can start as early as 9 years, especially where vaccination program entry is early, e.g., school-based programs.
Number of Doses (By Age)
If the series starts before 14 years of age:
2 doses, given 0-6 months apart (most adolescents).
If the series starts at 15 years or older (up to 26):
3 doses, at 0, 1-2, and 6 months.
Catch-up Vaccination (Older Adolescents / Young Adults)
Ages 13 to 26 (unvaccinated or not fully vaccinated):
Should complete the full series of 2 or 3 doses as per given above.
Ages 27 to 45 (selected adults):
Not routinely recommended for everyone; individualized decision after discussion with a doctor (considering prior exposure, risk, and cost-effectiveness).
Special Groups (Immunocompromised)
Children/adolescents 9 to 26 years who are immunocompromised:
Usually advised 3-dose schedule even if first dose is for <15 years because immune response may be weaker.
Key Points
- Best time: Before sexual activity begins, ideally 9 to 14 years, when the immune response is strongest.
- Gender: Recommended for both girls and boys to prevent HPV-related cancers and genital warts.
- Safety: HPV vaccines have an excellent safety profile; common side effects are mild (pain at the injection site, low-grade fever).
HPV Vaccine: Common Side Effects
Most side effects are mild and short-lived, appearing within a few hours to days after vaccination.
Very Common (Local Reaction)
Pain, redness, or swelling at the injection site (arm).
Common General Side Effects
Headache, mild fever, tiredness, and nausea. Muscle or joint pain, dizziness, or feeling faint.
Important Fainting (Syncope)
Fainting is more common among adolescents after any vaccine, including HPV; it is usually brief and resolves quickly. To reduce risk, providers often ask the person to sit or lie down for about 15 minutes after the shot.
HPV Vaccine: Serious Side Effects (Very Rare)
Scientific surveillance shows serious adverse events are uncommon and not clearly linked to the vaccine at higher rates than background levels.
Severe Allergic Reaction (Anaphylaxis)
Very rare; occurs within minutes and is treated immediately with adrenaline and medical care.
Large studies and post-marketing surveillance (VAERS, WHO-GACVS, and other registries) have not found consistent increases in autoimmune diseases (for example, multiple sclerosis and rheumatoid arthritis). Long-term neurological or chronic debilitating conditions causally linked to HPV vaccines.
HPV Vaccine: Safety Data and Evidence Base
CDC and WHO Position
Over 15 years of monitoring and many millions of doses show that HPV vaccines are safe and effective. No respected agency has found credible evidence that HPV vaccines cause infertility, autism, or systematic long-term harm.
Real-World Studies
(e.g., 18-year US safety analysis):
Reported adverse events are mostly non-serious (pain, dizziness, fainting-type reactions). The proportion of serious reports has declined across newer vaccine generations (e.g., fewer serious events within 9-valent Gardasil-9 than with older versions).
Benefit Far Outweighs Risk
HPV vaccines prevent many cancers like cervical, anal, penile, vulvar, vaginal, oropharyngeal, and genital warts.
For most people:
The HPV vaccine is highly safe; common side effects are mild and self-limiting. Serious events are very rare and respond well to prompt medical care.
Effectiveness of the HPV Vaccine in Preventing Cancer
The HPV vaccine is highly effective at preventing HPV-related cancers, especially when given before sexual exposure to the virus. Protection is strongest for cervical cancer, but it also reduces the risk of several other HPV-driven cancers.
How Effective Against Cervical Cancers?
In women vaccinated at a young age (before exposure to HPV), large real-world studies show the following:
About 85% to 90% reduction in cervical cancer incidence compared with unvaccinated women.
For girls vaccinated before age 17, studies report up to nearly 90% lower risk of invasive cervical cancer.
In clinical trials and analyses limited to people not previously infected with the vaccine types, the vaccines are close to 100% effective at preventing:
Persistent infection with the vaccine-type HPV.
High-grade cervical precancers (CIN ⅔, AIS) caused by those types.
Effective Against Other HPV-Related Cancers
The same high-risk HPV types, especially 16, 18, 31, 33, 45, 52, and 58 in the 9-valent vaccine, cause most cases of anal, vulvar, vaginal, penile, and oropharyngeal cancers.
Population data shows strong declines in precancerous lesions (anal, genital) and early signs of reduced rates of these cancers in vaccinated cohorts, though long-term cancer data are still emerging.
Key Points
Best Protection: Vaccination in early adolescence (ages 9 to 14), before first sexual contact, gives the highest cancer prevention effect.
Real-world impact: Countries with long-running school-based HPV programs, e.g., Sweden, the UK, and Australia, report dramatic drops in cervical precancers and cervical cancer in vaccinated cohorts.
Overall, HPV vaccines are one of the few tools that directly prevent cancer and, when coverage is high, can dramatically reduce the future burden of several HPV-related cancers.