Reproductive tract infections (RTIs) and sexually transmitted infections (STIs) represent a major global health challenge, with STIs alone causing over 374 million new curable cases annually, according to WHO estimates. RTI encompasses a broader category that includes STIs plus non-sexually transmitted infections.
Magnitude of STI Disease
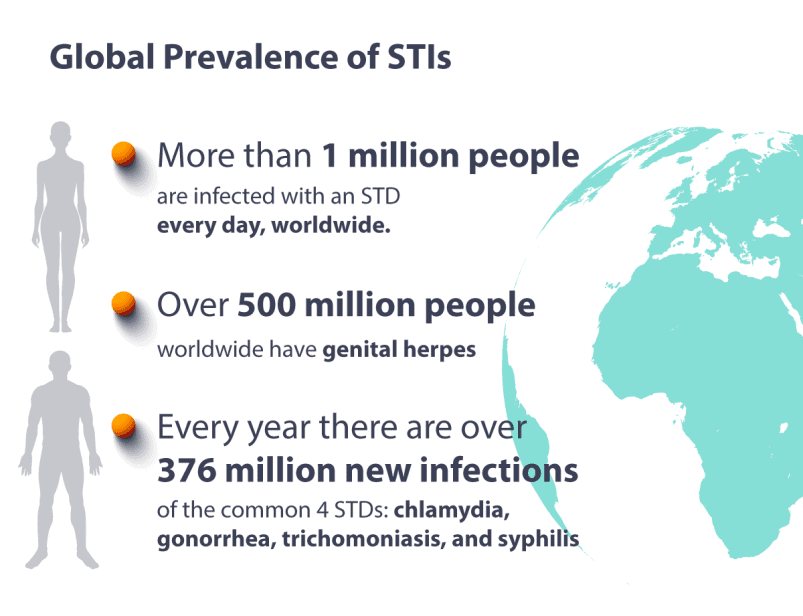
Sexually transmitted infections (STIs), also known as STDs, affect millions globally each year, with over one million curable cases acquired daily among people aged 15 to 49. STIs like chlamydia, gonorrhea, syphilis, and trichomoniasis drive much of the quantified burden, with 2020 WHO data showing 129 million chlamydia, 82 million gonorrhea, 7.1 million syphilis, and 156 million trichomoniasis cases worldwide. Incident cases rose to nearly 770 million globally in 2019 for five common STIs (excluding HIV), with China and India reporting the highest absolute numbers. Over 1 million disability-adjusted life years (DALYs) in 2021.
Magnitude of RTI Disease
RTIs include endogenous infections, e.g., bacterial vaginosis and candidiasis, alongside STIs and iatrogenic ones, but global prevalence estimates are less centralized than for STIs. Studies indicate RTI symptoms affect 42% to 90% of women in regions like Southeast Asia, though lab-confirmed rates are lower (e.g., 9.7% in one center). Non-STI RTIs like yeast infections are common even among women, often exceeding STIs in certain populations due to factors like hygiene or hormones.
Global Burden Summary
South Africa faces the world’s highest STI burden due to intertwined biological, socioeconomic, and behavioral factors amplified by its HIV epicenter status. High HIV prevalence creates a vicious cycle, as STIs like gonorrhea and chlamydia cause genital inflammation that triples HIV acquisition risk, while HIV weakens immunity to foster STI spread.
The combined RTI/STI burden leads to infertility, ectopic pregnancy, chronic pain, and increased HIV risk, with the highest rates in sub-Saharan Africa and developing regions. In 2021, STIs (excluding HIV) caused over 722 million incident cases and 7.9 million DALYs globally, while RTIs amplify this in low-resource settings. Control efforts focus on STI screening due to better data, but RTI prevention requires broader hygiene and healthcare access.
Systemic Challenges
Poverty limits healthcare access, with fragmented screening missing asymptomatic cases. Antimicrobial resistance in gonorrhea, inadequate sex education, and historical surveillance gaps hinder control, despite syphilis declines from better maternal services.
STI vs RTI Differences
| Aspect | STI | RTI |
| Transmission | Primarily sexual contact, blood, or perinatal | Sexual STIs, endogenous overgrowth, or medical procedures |
| Examples | Chlamydia, gonorrhea, syphilis, | Bacterial vaginosis, yeast infections, and STIs |
| Scope | Subset of RTIs, often asymptomatic | Broader genital tract infection is common in women. |
| Global Data | Well-tracked, e.g., 374 M cases/year | Higher prevalence but less quantified |
Highest Burden Countries for STIs and RTIs: China and India
China and India bear among the highest absolute burdens of STIs/RTIs globally due to their massive populations, alongside countries like Indonesia and Nigeria. China leads with over 148 million estimated STIs/RTIs cases in 2021, driven by high population density and urban migration patterns. India follows closely with about 94 million cases, reflecting challenges in screening and rural access.
High DALYs Burden
South Africa tops disability-adjusted life years (DALYs) at nearly 59 million, followed by Nigeria (4.6 million) and India (3.25 million). These metrics highlight not just cases but also long-term health impacts like infertility and chronic complications.
Southern African nations dominate rates per 100,000: South Africa (39,598), Lesotho (40,747), Eswatini (38,608), and Botswana (38,456). China and India rank higher per capita (e.g., India at ~7,858) but overwhelm in totals.
Prevention Strategies For STI and RTI Globally
Global prevention strategies for STI and RTI emphasize integrated health services, education, and access to tools like condoms and diagnostics, as outlined in WHO’s 2026 operational handbook. These approaches aim to reduce over 1 million daily new STI cases while addressing RTI through broader hygiene and endogenous infection control.
Primary Prevention
Safe sex practices, including consistent condom use and fewer partners, form the cornerstone for both STIs and RTIs. Vaccination against HPV and hepatitis B and C prevents key STIs, while RTI strategies promote hygiene, proper underwear, and pH-balanced products to curb endogenous infections like bacterial vaginosis. Education campaigns target high-risk groups, integrating STI/RTI awareness into HIV, maternal, and adolescent health platforms.
Screening and Treatment
Routine screening via syndromic management and rapid diagnostics catches asymptomatic cases early, with partner notification ensuring contact tracing. WHO recommends antimicrobial stewardship to combat resistance, alongside doxycycline post-exposure prophylaxis for high-risk populations. RTI treatment focuses on antifungals or antibiotics for non-STI causes, emphasizing primary care integration.